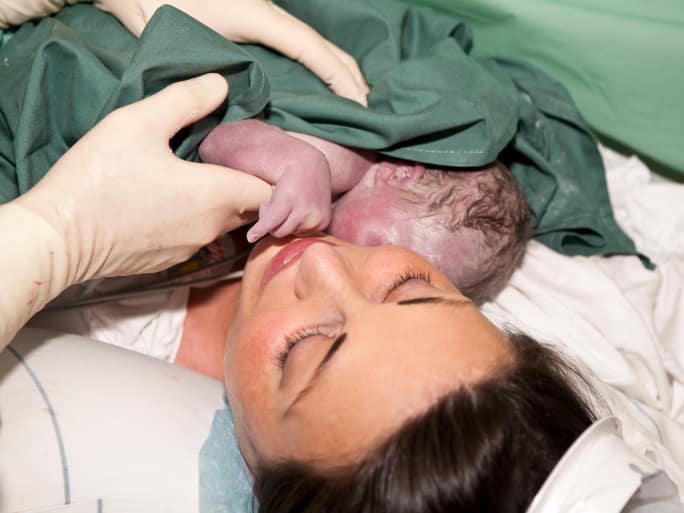
I’m So Happy I Didn’t Let My Doctor Talk Me Into Having A Second C-Section
 Leah Marshall originally wanted a vaginal birth for her first baby. But like a lot of first-time mommies, she encountered several problems during delivery that ultimately did lead to an emergency c-section. Her baby turned out to be quite large, weighing nine pounds and six ounces and positioned “sunny side up” causing her cervix to swell up instead of open. Her contractions were also very abnormal with “double peaking,” even after the pitocin arrived. Leah tells me that at the time, doctors were unaware that all of these factors were perhaps caused by her son’s size, his positioning, or a combination of both.
Leah Marshall originally wanted a vaginal birth for her first baby. But like a lot of first-time mommies, she encountered several problems during delivery that ultimately did lead to an emergency c-section. Her baby turned out to be quite large, weighing nine pounds and six ounces and positioned “sunny side up” causing her cervix to swell up instead of open. Her contractions were also very abnormal with “double peaking,” even after the pitocin arrived. Leah tells me that at the time, doctors were unaware that all of these factors were perhaps caused by her son’s size, his positioning, or a combination of both.
After a successful c-section brought her son into the world, Leah’s doctors suggested that she default c-sections on all future additions to her family. But even though vaginal birth carries some risks following an initial c-section, Leah committed to a VBAC (vaginal birth after c-section) to achieve the birth experience that she wanted.
When Leah became pregnant with her second baby, she started to experience many of the uncomfortable symptoms she remembered with her first pregnancy. During both pregnancies, she suffered from severe inflammation and pain in her public symphysis, which was relieved by routine visits to a chiropractor.
“[With my first pregnancy], I was often unable to walk more than from the couch to the bathroom, and I knew that would never do when I had a preschooler to chase as well,” she remembers. “The chiropractor believed that whatever structural abnormalities led to my pain probably impacted my labor.”
Leah describes her general practitioner as “disapproving” of both her choice to attempt a VBAC but also her interest is seeking out midwives for her prenatal care. Her mother-in-law, a labor and delivery nurse for over 20 years, also initially expressed concern, convinced that Leah was unaware of the risks. There was also the assumption from friends and acquaintances that she was “some sort of deluded hippie feminist” for taking an active decision in her birth.
“While I am often deluded, have a few hippie tendencies, and am certainly a feminist, I am also a fairly typical suburban mom,” she says. “Mostly the attitude seemed to be that was I taking a ridiculous risk, and I should just trust that the doctors who wanted me to have a second c-section knew better. And while I was really committed to a trial of labor, I can’t claim that as my due date drew near, I wasn’t terrified that I was making a terrible decision.”
After a big family move to Tucson, Arizona, Leah asked around for a highly recommended midwife, eventually arriving at “the only show in town for VBACS.” The midwives informed Leah of the same risks: a low, but documented chance of uterine rupture and severe bleeding. While doing her research, she was horrified to discover that even the midwives didn’t share with her the medical risks of having two or more c-sections. Leah’s delivery nurse mother-in-law expressed little worry about the omission, telling her that many doctors often don’t feel the need to share this information with their patients given how much smaller modern families are.
“I don’t think that justifies failing to inform women,” says Leah. “The size of my family shouldn’t be decided for me. It’s enough to make me think maybe doctors are pushing c-sections because it’s easier on their schedules.”
Finally, the day of Leah’s delivery came. For insurance purposes, her labor had to be scheduled at a hospital rather than at a birthing center. Her midwife was in attendance as Leah struggled through pain and frustration with little to no progress. Her midwife found that she was already five sonometers and several attendees weighed the option of going for another c-section. The baby’s head was noticeably stuck, just like that of her older son during her first labor. Leah’s midwife did one last inspection before calling the doctor. She determined that the infant’s head had gotten caught on the edge of her cervix and after some maneuvering, Leah found herself pushing. The epidural wore off at what she calls “just the right time,” as she had been numbed during the worst part of labor while now experiencing the final push of her second baby.
As for surprises in her VBAC experience, Leah says that she was completely unprepared for how much easier her recovery was as opposed to a c-section recovery. In particular, she noticed that she eased right back into her sex life without much complication.
“After experiencing both, I can’t even imagine volunteering to have a c-section. Probably the most surprising difference for me was that the return of normal sexual function was much easier too. I had lots of pain when restarting sexual activities after my c-section.”
A few years later, Leah is absolutely certain that she made the correct decision for herself and her family. Now that her second son is leaving his toddler years, she and her husband are considering a third baby, a possibility that isn’t framed in potential c-section risks. She envisions her birthing choice as a political one in a health system that, according to her, “still treats women as second-class citizens.”
At the same time, she fully acknowleges that not all women can achieve the same birthing options that she so fiercely sought out for herself.
“My own experience comes from a place of great priviledge. My health insurance, location, and education allowed me lots of choices that many women don’t have.”
She adds, “Too often we allow the conversation about women’s health to be reduced to a battle over abortion rights when there are lots of other ways in which our rights and choices are slowly being eroded away.”
(photo: Leah-Anne Thompson/Shutterstock.com)